Burning for bleeding peptic ulcers
Burning for Bleeding Peptic Ulcers
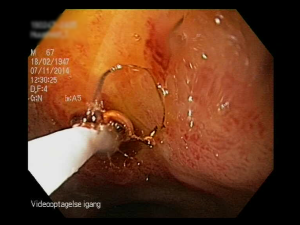
Researchers from the University of Southern Denmark (SDU) and the Department of Medical Gastrointestinal Diseases at Odense University Hospital (OUH) are involved in several research projects that branch out worldwide to other research centres. The goal is to optimize and improve the treatment of bleeding peptic ulcers, which occur especially in older people.
Over the past few years, the Department of Medical Gastrointestinal Diseases has treated patients using an apparatus that only four other centres in the world use (two in the United States, one in Hong Kong and one in Germany). The Doppler apparatus can detect whether there are blood vessels hidden under a peptic ulcer. If there are, there is a risk that the ulcer will burrow into the blood vessel and cause further bleeding.
– We use the Doppler after keyhole surgery, which is the preferred treatment method. But in one out of eight patients, the wound breaks open again. If this happens, the risk of death is five times higher, says medical doctor and researcher Stig Borbjerg Laursen.
A ticking time bomb
Doctors cannot predict which patients will experience the extra bleeding, and it is here that Doppler has its strength.
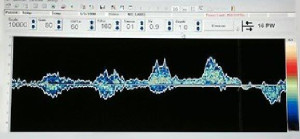
– It works in the same way as sonar when fishermen are looking for fish in the sea and can see on a screen whether there is any life under the surface. If there are no fish, there is just a thin, straight line on the screen. It is the same with our new apparatus, which can measure at a depth of only one millimetre using a thin tube at the surface of the ulcer. If the doctors can see a blood vessel that is placed like a ticking bomb, they can use a heating device at 280 degrees to burn the whole wound bed to prevent bleeding. The Doppler is then used again to check the result. This is all done as part of a worldwide study to assess the effectiveness of the Doppler apparatus, with OUH the only Scandinavian hospital in the study.
All patients with bleeding peptic ulcers or suspected underlying blood vessels are invited to participate in the study, and every second patient receives the extra Doppler intervention.
A tube through the groin
About 50% of bleeding peptic ulcers are treated with medication, and the other 50% with keyhole surgery. But in one out of ten patients, the ulcer bleeds so strongly that keyhole surgery cannot be used. In these cases, the radiologists at OUH take over (at any time of day or night) and insert a small plastic tube in through the groin and up through the blood vessels to the site of bleeding, where they place titanium wires inside the blood vessel. This can stop the bleeding in about 95% of patients.
This method (embolization) is less invasive and side effects are rare. It is a great advantage for older patients, of whom about half also have heart disease that must be taken into consideration, says Stig Borbjerg Laursen. The department showed in an earlier study that mortality after embolization is lower than after traditional surgery for bleeding peptic ulcers.
Data from several thousands of patients
Professor Ove B. Schaffalitzky de Muckadell emphasizes that having relatively few patients to treat does not prevent research. Several research projects have been started up and they will add to the existing knowledge about how to optimize treatment.
– The newest big study is one that we are doing in collaboration with centres in the US, Scotland, England, New Zealand and Singapore. This allows us to collect data from several thousands of patients each year, and sharing of the results will benefit patients around the whole World.
Administration of blood and fluids before surgery
Since 2004, the treatment of all patients admitted to Danish hospitals with a bleeding peptic ulcer has been recorded as part of the Danish Regions’ clinical quality development program. This database contains data on about 20,000 Danish patients.
– When we compare ourselves with other hospitals, OUH does extremely well, says Ove B. Schaffalitzky de Muckadell.
– Our success is partly because we can offer the latest treatments, but also due to the treatment that the patients have received in the Emergency Department (FAM), prior to admission to our department.
– Our collaboration with FAM means that we receive stable patients with good blood and fluid balance. The goal is not to close the bleeding ulcer as quickly as possible. The survival rate increases when the patient is well prepared for the surgical procedure to be undertaken in our department.
The first with special patient rooms
The good results have not come out of the blue. Over 30 years ago, OUH was the first hospital in the country to provide special rooms for patients under observation for potential bleeding of peptic ulcers. Special rooms for this type of patient are still rare in Danish hospitals.
– The doctors and nurses attached to these rooms are specially trained to identify the alarm signals for a bleeding ulcer, so they can intervene very quickly. An English study has shown that the mortality rate is lower if patients are treated in a special section of the gastrointestinal department, rather than sharing a room with patents with other diagnoses in a general admission ward, says Ove B. Schaffalitzky de Muckadell.
FACTS
What causes peptic ulcers?
In three-quarters of cases, ulcers in the stomach or duodenum occur as side effects to painkillers used for arthritis, or medicines that contain acetylsalicylic acid (aspirin). The other one-quarter of ulcers occur due to bacteria in the stomach that have ben present since childhood. The bacteria usually cause ulcers later in life, when the stomach is less able to produce protective factors.
Each year, the Department of Medical Gastrointestinal Diseases offers nationwide courses for doctors and nurses to disseminate the latest research results in the treatment of bleeding peptic ulcers.
MORE INFORMATION?
 |
Ove B. Schaffalitzky de Muckadell, Professor, Department of Medical Gastrointestinal Diseases Mail: sdm@rsyd.dk |
 |
Stig Borbjerg Laursen, Department of Medical Gastrointestinal Diseases Mail: stig.laursen@rsyd.dk Telephone: 30207859 |

